HFrEF: A Challenge We Can Overcome
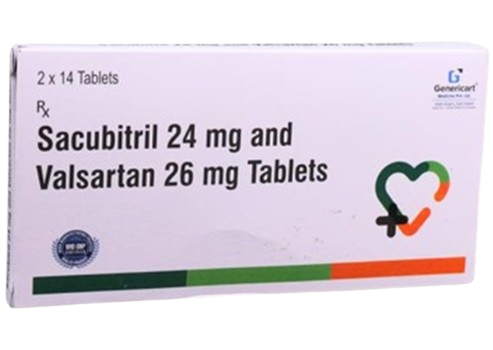
Guideline-Directed Medical Therapy (GDMT) is transforming the management of Heart Failure with Reduced Ejection Fraction, offering a proven roadmap to improve patient outcomes — yet adoption remains suboptimal.
Ref: JAMA Cardiol. 2024;9(4):397–404